Take Back Your Skin (Part 2): Tell Your Story
If I could write this post in three words, they would be the following: eczema is psychosomatic. I’ll repeat that in bigger lettering to emphasize how important it is:
ECZEMA IS PSYCHOSOMATIC.
What do those three words mean? The short version is that eczema can be triggered or exacerbated by anxiety, stress and depression. The long version is spelled out below.

Now Take it Back is reader-supported. When you purchase through links on my site, I may earn an affiliate commission at no additional cost to you. All opinions are my own. See my full affiliate disclosure for more information.
eczema is psychosomatic
Anyone who suffers from eczema intimately understands the link between eczema and mental health. Eczema can radically damage self-esteem, or, in extreme cases, contribute to outright self-loathing. The cyclical nature of periodic breakouts followed by temporary recovery can be particularly detrimental to psychological well-being, leading to feelings of hopelessness.
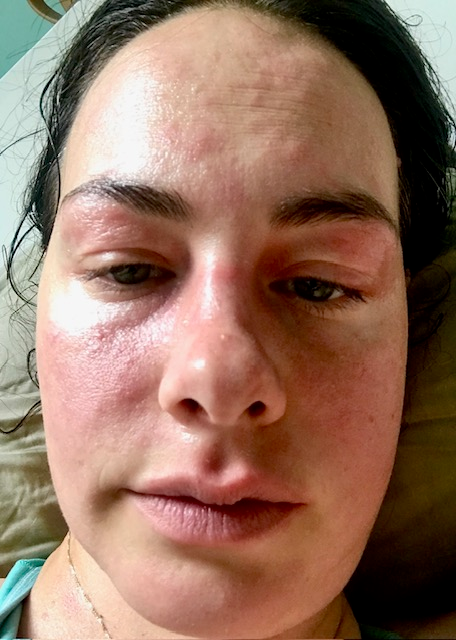
Eczema is an unavoidably obvious disease; it is difficult to conceal bright red, weeping, bleeding or bandaged portions of skin. Broken skin draws attention, causing humiliation and shame, triggering the desire to hide. The need to communicate that this disease is not contagious is acute; the compulsion to apologize for subjecting others to broken and bleeding skin is all-consuming.
Those who suffer from eczema often feel that eczema controls how they see themselves as well as how others perceive them. They feel like eczema controls where they can go and what they can do. They feel like no one will ever want to engage in an intimate relationship with them. Eczema is a tyrannical master.
does eczema cause depression?
Atopic dermatitis (eczema) has a long history of being associated with depression, anxiety and attention-deficit hyperactivity disorder (ADHD). It is moreover known to damage sleep quality and thereby impact mental health.
Among the social impacts of atopic dermatitis are difficulties and detachment in relationships and social stigmatization. Additionally, atopic dermatitis is known to cause sleep disturbance, anxiety, hyperactivity, and depression.
– Frontiers in Immunology (2024)
A meta-analysis published in the American Medical Association’s Dermatology Journal found that patients with atopic dermatitis (the medical term for eczema) were 44% more likely to exhibit suicidal ideation and 36% more likely to attempt suicide compared with patients without atopic dermatitis.
The National Eczema Association states that managing stress and improving sleep quality is essential to eczema treatment. Such practices as personal or group talk therapy, gentle exercise, taking up a hobby, or building relationship with a pet are highly encouraged methods of managing stress.
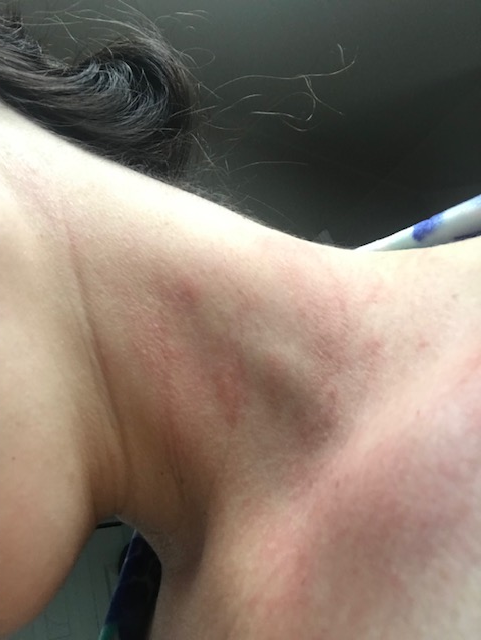
does eczema cause social isolation?
Atopic dermatitis (eczema) has a long history of being associated with significant social stigma. Children who develop eczema often experience teasing and bullying, leading to a poor self-image, exacerbation of symptoms and a tendency to avoid social environments.
Atopic dermatitis showed positive associations with self-reported chronic fatigue syndrome, burnout, depression, social phobia, panic disorder, attention deficit hyperactivity disorder, and eating disorder in the participants’ lifetimes.
The “psychosocial” burden of eczema is significant and well-documented. Atopic dermatitis alone can cause new depression and anxiety, which increases in severity according to the severity of the eczema.
does eczema cause shame?
Science has accumulated an extensive library of academic proof that people with atopic dermatitis struggle with psychological comorbidities. These highly respectable practitioners will tell you that people with atopic dermatitis experience feelings of being unable to enter into relationships–especially intimate relationships–because of eczema.
But to truly explore the intimate relationship between eczema and shame, you need to talk to someone who has actually suffered from it. To talk about eczema’s relationship with shame, self-loathing, depression, anxiety and loneliness, I need to tell you my story.
my eczema story
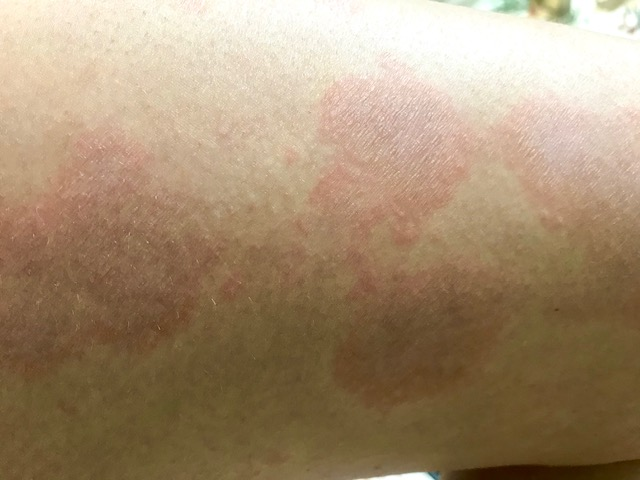
I’m told I developed eczema as an infant. My earliest memories include watching my siblings eat fresh strawberries and not being allowed to because I had eczema. In middle school, I would come home from soccer practice with large patches of skin on my inner elbows and knees bright red and swollen from cold air exposure.
My friends gently mocked me for my medicated Blistex addiction; my lips and the skin between my lips and my nose were always coated and shiny with Blistex. The mentholated goop felt cooling to my constantly inflamed skin and the petroleum-like substance provided a psychological and physical barrier from any potential irritants that could make my lips worse.
The skin between my lips and nose would not heal no matter what skin care products I tried. Throughout adolescence, I applied and reapplied hydrocortisone cream to that stubborn patch above my lips. I slathered it on my inner elbows, inner thighs and the swollen and painful backs of my knees.
hormone disruption
By the time I turned 15, my bra size was somewhere in the E/F zone. My parents tried to gently tell me that the hydrocortisone had impacted my hormones and caused my breasts to grow too large. I grew more and more self-conscious, wearing baggy shirts and hunching my back to try to hide the size of my breasts.
Eventually, my parents decided a breast reduction would improve my self-esteem. The cosmetic surgeon assured us that he would be using the best liposuction technology available, and I should be able to breastfeed if I ever decided to become a mother one day.
I spent the weekend after the surgery draining fluids into bags attached by tubes to the surgical holes beneath my armpits. For several years following the surgery, the horseshoe-shaped scar tissue in my breasts needed to be massaged constantly to encourage my lymph nodes under my arms to drain properly. Two years out from the surgery, I needed a mammogram to make sure the scar tissue wasn’t providing a breeding ground for breast cancer.

seborrheic dermatitis
Meanwhile, the dandruff on my scalp grew so bad that other students sniggered behind my back as huge white flakes of my skin fell onto my desk and the floor around me at school. I went through bottle after bottle of medicated shampoo trying to heal my scalp and curb my humiliation. My Friday night trips to Walmart always included me purchasing my skin care staples: moisturizer, lip balm and hydrocortisone.
At the recommendation of an endless parade of dermatologists, I tried every skin care company on the market. Natural remedy attempts included jewelweed, castor oil, peanut oil, olive oil, coconut oil, eucalyptus oil, and a wide range of essential oils.

chemical sensitivity
I attended undergraduate college at a small liberal arts school on the eastern shore of Maryland, right in the heart of state agricultural land. A brief comment during orientation noted that we should try to buy bottled water whenever possible because the pesticide runoff from the local farms polluted the local water supply. I didn’t realize how much drinking and showering in this high-chemical water would affect me until the eczema had spread to cover my entire back, shoulders, and buttocks as well as my ankles, wrists, neck and the thin skin surrounding both of my eyes.
My skin care rituals included using a butter knife to relieve the endless, ever-increasing, insanity-inducing itchiness that covered my legs. After scratching until I bled, I showered in the hottest water I could stand, directing the flow of the almost-too-hot water to scald patches of unbearable itchiness on my wrists and back, trying to let the hot water scratch for me without further breaking the skin.
Itching my eyes in the shower always made them so swollen that I had to remove dry and crusted puss the next morning to open my eyes. With every shower, I swore to myself that I would never again itch my eyes in the shower. Yet, inevitably, the hot water on my face caused such unbearable itching that I would break down, and for a few blissful moments, scratch and rub my eyes until the skin was once again broken and seeping.

pain management
Every night before bed, I bathed my body in castor oil, the only substance that was thick enough to coat and somewhat seal the thousands of micro-wounds covering my body. Each year, I went through several pairs of castor-oil-laden sheets that were greasy and heavy with absorbed oil. I threw away more than ten pairs of sweatshirts and sweatpants that stank of castor oil, no matter how many times I washed them in baking soda and high-efficiency detergent.
Mornings were best for me. My skin would invariably heal a small amount as I slept, but the act of waking and going about my day would irritate and trigger the eczema, until, by bedtime, my skin was typically a tiny amount worse than it had been the previous night.
Wound care took up a lot of my time. I started to use sterile bandages, tape, gloves and adhesive bandages for the smaller patches. Coworkers at my summer jobs joked that I looked like a mummy because I showed up for work with my wrists and my ankles slathered, bandaged, then wrapped in oil-soaked elastic bandages.
I spent a semester abroad in Cork, Ireland and traveled with my best friend to Italy, England, France, and Portugal. Our luggage was lost on our flight to Finland during one particularly brutal eczema breakout. I was stranded for a week in beautiful and clean Helsinki with swollen and burning skin and without hydrocortisone, castor oil and clothes. We asked our hosts where to find a local anti-itch cream, bought some clothes, and spent the week reassuring many kind strangers that my face was swollen and red from a skin problem and not because I was crying.

natural remedies
By junior year of undergraduate, I had started to do my own research on the causes of eczema. My roommate and I shared a tiny apartment across the street from the local health food store. I started buying their 5 gallon jugs of purified water and hauling them across the street to our apartment several times a week. I started to use the cafeteria less and purchase groceries from the health food store. I did a colon cleanse and went through Alcat food sensitivity testing. I started taking supplements. It felt good to be proactive about my health, but my eczema didn’t improve.
Throughout my senior year, I continued my research into the world of health self-help. I tried to teach myself how to cook and struggled with portion control and using whole ingredients. The summer after I graduated, my cousin told me he was following the neanderthal/paleo diet to alleviate symptoms of his type 1 diabetes. He said he thought the paleo thing worked well for our genetics, so I gave it a try.
In a little over 3 months, I dropped the 50 lbs I had gained steadily throughout my undergraduate career. My eczema improved but didn’t disappear. I felt thin and confident, perhaps for the first time in my young life. I started graduate school in Washington, D.C. and tried to stick to paleo diet principles. My eczema returned with the winter.

gut dysbiosis
For the next 7 years, while I finished graduate school, started a career as a teacher and got married, my eczema followed a very distinct pattern:
- It improved during the summer and worsened during the winter.
- It improved when I dropped weight and worsened when I gained weight.
- It worsened during periods of high emotional or physical stress.
I was 29 when I started to develop chronic and severe stomach pain/cramping. Other symptoms included nausea, dizziness, tachycardia, fainting, constipation and diarrhea. The human resources manager at work suggested I might be pregnant. My gynecologist diagnosed me with unexplained infertility. My cardiologist ungently suggested that I get in shape. My gastroenterologist stuck a camera down my throat to look at my stomach but didn’t find anything unusual. My uro-gynecologist prescribed me with a daily antibiotic to manage my chronic urinary tract infections.
I quit my job. I started taking a high-dose probiotic every day. I did another colon cleanse and a juice fast. I started gardening, landscaping my yard, and generally being outdoors more and sleeping more. Within a year, I was pregnant with my first daughter.
dyshidrotic eczema
Pregnancy hormones suppressed my eczema. Instead of constantly bandaging my skin, I spent nine months nauseated on the couch, researching birth options and how to breastfeed after a breast reduction. My eczema and stomach pain returned full-force roughly six months after my first daughter was born and the pregnancy hormones started to leave my body. My daughter’s first toys included the paper wrappings from the countless boxes of adhesive bandages used for wound care on my fingers.
My hands were wrapped, mummy-style, during her first birthday to manage pain and infection. The eczema had inexplicably worsened after my pregnancy and was raging out of control on the backs of my hands and all over my fingers. I went through box after box of nitrile gloves, trying to keep up with caring for an infant, cooking, cleaning, and gardening.
Day after day, I would apply over-the-counter antibiotic ointment or hydrocortisone to the worst patches on my fingers, wrap the wounds with adhesive bandages, coat the remaining skin on my hands in coconut or castor oil, put on a pair of nitrile gloves, then put on dish gloves or gardening gloves to do my work.

the burden of disease
This managed pain and prevented further irritation quite effectively, but the eczema was rarely exposed to air and never dried out. Sometimes, the sweat from long hours spent in nitrile gloves increased swelling and itchiness, and the patches would become infected and spread from finger to finger.
Ironically, if I was sick with a respiratory or gastrointestinal virus and stayed in bed for a few days, the eczema improved radically. This created quite a conundrum; if I did nothing with my hands, my eczema would improve, but if I used my hands, my eczema would worsen, and I would need to spend more time on wound care.
I worked diligently to try and time everything precisely so that I could care for my daughter first, myself second, then still have time to wrap my hands—without my daughter getting overtired and beginning to scream at me. I did my best and failed more often than I succeeded.
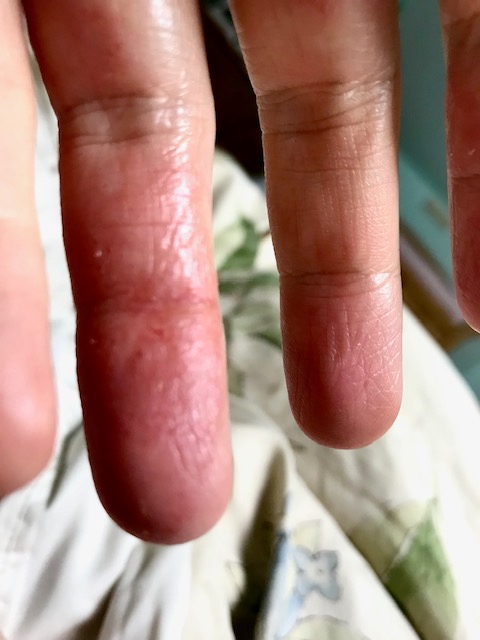
the gut-brain axis
My sister recommended that I read a book called Gut and Psychology Syndrome by Natasha Campbell McBride, since it proposed a solution to both my eczema and my stomach pain. I began the GAPS diet shortly after my daughter turned one.
I tried to teach myself how to make sauerkraut, bone broth, and butternut squash pancakes within the course of one week and ended up in hopeless tears.
Over the next 5 months, I followed the general principles of the GAPS diet very loosely and ended up losing over 50lbs of weight that had accumulated throughout the 7 years of working and becoming pregnant. I felt healthy and happy again and dreamed of all the places I wanted to show my daughter one day.

The very worst time with my eczema occurred shortly after this, during my divorce. My hands needed to be constantly wrapped, and I developed a MRSA infection in my leg from not cleaning a wound I had viciously scratched on my calf muscle while packing out my house. I needed to switch antibiotics to control the infection and take a separate course of antibiotics to fight the urinary tract infection that was happening simultaneously.
The next year of my life was a nightmare for many reasons, and the state of my mind and heart was reflected on my skin.
from victim to agent
It wasn’t until my second daughter turned one that I really made the decision to find a way to manage my eczema once and for all. I scoured the internet for success stories, management techniques or some elusive super-secret solution to the disease that had plagued me for my entire life.
I came across a woman in Australia who had built a career counseling people about eczema; I tried her diet. I began seeing an integrative physician who recommended I do bloodwork for another round of Alcat testing. My food sensitivities came back completely different from those I had tested positive for in college. I found a mom blogger who had healed her kids’ eczema using a program called Gut Thrive in 5; I completed this program.

I did bone broth fasts, celery juice diets and parasite cleanses. I went on daily walks and bike rides with my daughter and tried to get as much sunlight as possible. I did coconut oil pulling, detox baths and home enemas. I taught myself how to make staple foods from scratch and tried to adapt my favorite recipes to healthier versions.
food as medicine
I devoured anti-carb, grain-free cookbooks and cooking blogs and gorged on nutrition podcasts. I finally came across a program with Institute for Integrative Nutrition and completed their health-coach training program.
Over the course of two years, I taught myself to be completely fixated on health and obsessed with following principles I had learned from the GAPS diet and the Gut Thrive in 5 program. I pressured those around me to eat and cook the way I did. I was the thinnest and healthiest I had ever been, and I felt like I had found the answers. I was an evangelist for health.

And my eczema was gone. Well, mostly. It still came back in the winter—a little bit. Or if I had too much alcohol or sugar. Or if I was really stressed or angry. Or if I didn’t get enough sleep. But it was only on my hands and sometimes on small parts of my arms.
I didn’t want to acknowledge the limitations of my diet and lifestyle changes. I WANTED diet, exercise, and environmental factors to be the solutions to eczema. I finally felt like I could control those aspects of my life. And changing my diet, exercise, and environmental factors had improved my overall health and my eczema more than anything else ever had.
But I still had breakouts.
making room for mystery
In 2022, I married my husband. Over the past 3 years, we have had two beautiful little girls together: my third and fourth daughters. The time has passed in a whirlwind of pregnancies, births, homeschooling, blending families and choosing profoundly IMPERFECT diet and lifestyle choices.
And somehow–in all that constant and unending almost 4 years of chaos–I have not suffered from eczema breakouts.
I could try and pretend like I have the answers, but I don’t. Life, breath and love are too mysterious to possess or dominate. I don’t pretend to have secret knowledge about how to heal eczema because I don’t really know anything.
But I was 35 years old before I felt truly loved and secure in an intimate relationship. For almost 4 years, I have been able to wake up from nightmares, reach for my husband’s hand and immediately feel safe. I have 3 beautiful, breathing daughters worth every ounce of my will to live. And, although I have more physical and psychological wounds than I can number, I am finally–imperfectly–home.

telling your story
Eczema is psychosomatic.
Telling your story—especially to yourself—can help you in ways than a food diary never will. This disease is, after all, multi-factorial. It is caused by so, so, SO much more than what you eat. To battle eczema, you MUST confront your mental health. And the easiest way to start is to tell your story.
why I don’t recommend food diaries
Dermatologists, nutritionists, allergists, and health coaches alike have suggested to me that I try an elimination diet and/or keep a food diary. Here’s why elimination diets and food diaries didn’t work for me:
- I quickly fell out of practice of documenting what I ate every day.
- I avoided my food diary when I felt guilty or ashamed of food I had eaten.
- It felt impossible to determine if food or stress was causing the breakout.
- I didn’t see an immediate payoff, so I lacked motivation to continue.
- It became just another thing that made me feel hopeless about eczema.
Despite these realities, I understand why so many practitioners recommend writing down your food habits. It helps with accountability, and it may help identify particular triggers. For example, I once tried a highly recommended vitamin C cream from a practitioner that I respected. The cream worked wonders for her, but it contained a soy-based carrier oil. It only took 1-2 days of applying this cream to my eczema patches to determine that I was highly allergic to soy. My eczema raged out of control within 48 hours of using the cream and didn’t calm down for weeks.

why telling your story will help
If you have eczema, you understand that no one knows how to heal you. You understand that you are the only person in existence that can heal yourself.
On your bad days, you may feel that your eczema story is a tragedy, and you are its victim. On your good days, you may choose to be the hero and fight even when it feels pointless to do so. It’s your eczema story, and you’re writing it page by page and day by day.
To help with this, I’ve created a free, printable PDF that breaks down the process of telling your eczema story. My recommendation is to use the prompts to write down your story at least once. No one needs to read it except for you. But writing down your battle with eczema can empower you to:
If you can write your eczema story every 3-6 months, you will have more data helping you track patterns over time. If you only write it once, you are guaranteed to learn more about your eczema than you knew before.
If you struggle with writing, ask someone you love and trust to be your transcriptionist—to ask you each question and type out your answer without any commentary. This is where you start addressing the connection between eczema and your mental health. You can download the pdf below:
why you still need to make space for mystery
At the end of my eczema journey, I was desperate to believe that diet and lifestyle changes were the whole story. I needed to believe that the sheer amount of money, work and suffering I had put into healing my eczema was worth it. I didn’t want to acknowledge my own limitations and how little I actually knew about my own body.
The most powerful lesson I took away from my health coach certification with the Institute for Integrative Nutrition was that health is far more comprehensive and complicated than diet and lifestyle. There is so much that science does not yet know about the interaction between the body and the mind, the pathogenesis of disease and the limitations of modern medicine.
Science does not like to make space for mystery.
I don’t like to either. But—because my eczema was caused by many more things than what I eat and what touches my skin—I was forced to accept the limitations of my understanding. Despite my perfect, strictly regimented diet and lifestyle, my eczema stayed with me. It wasn’t until I started to let go of control and surrender (at least a little bit) that my eczema retreated into a state of dormancy.
My mental health is still a daily struggle. I think it always will be. Most days, I try to make it very simple by attempting to follow three principles. I share them below in the hope that they can be as useful to you as they have been to me.
principles to live by
- YOU are the only person you can change; do not waste time and energy thinking or talking about how someone else should change.
- Pursue your joy; spend your free time thinking and talking ONLY about ideas and projects that excite and motivate you.
- Take responsibility for your life; choose to be the hero and NOT the victim of your own story.
becoming an agent
If you’re anything like me, eczema is only part of the picture of your poor health. At one point, my suffering included unexplained infertility, severe gastrointestinal pain, chronic bacterial infection and crippling depression. I had to reach a mental breaking point before I could choose to change enough things about my life to radically improve my health.
To read more about how to decide to stop being a victim to poor health and start to intentionally change your life, read Take Back Your Health (Part Two): From Victim to Agent.
Eczema is a complex disease; there is no one answer as to how to heal it. But there IS a path forward if eczema is corrupting and controlling your life. Diet and lifestyle changes can go a long way towards healing and resolving gut dysbiosis and immune dysfunction. But you must first reduce your chemical exposure before you can even summon the energy or the hope to try to change your life.
And–second– you must tell your story. You must tell it to make sense of what is happening to you. You must tell it because once you name something, you have some control over it. You must tell it because telling your story will also tell you what steps you need to take next to take back your skin.

take back your skin
This blog is about taking back control over your body and your life. I’m currently working on an ebook entitled Take Back Your Skin that details the exact steps I took to gain control over my eczema.
For updates on when this ebook will be released, please subscribe below!
Meanwhile, feel free to browse around for real-food recipes, self-care inspiration and some blunt honesty about preserving your mental health while parenting. There’s also some great freebies to take advantage of — check them out below!
take my free 5-day challenge
& instantly access: